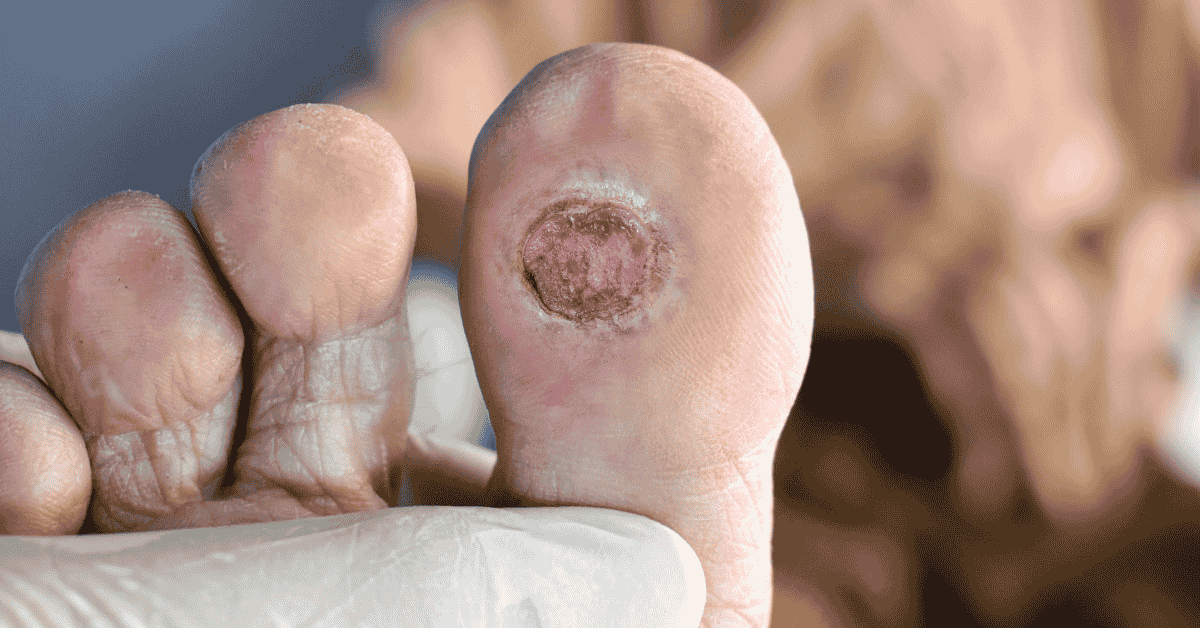
For people living with diabetes, foot health is more than a comfort issue — it’s a critical part of overall health. One of the most serious and common complications of diabetes is the development of diabetic foot ulcers, open sores or wounds that form due to a combination of nerve damage, poor circulation, and delayed healing.
What makes diabetic foot ulcers especially dangerous is that they often start small and painless, allowing them to go unnoticed until they become severe. Recognizing the early warning signs can help prevent infection, hospitalization, and even amputation.
Diabetes affects the body’s ability to heal in several ways. Over time, high blood sugar levels can damage nerves, a condition known as diabetic neuropathy. This reduces sensation in the feet, meaning cuts, blisters, or pressure points may not be felt at all. At the same time, diabetes can narrow and harden blood vessels, limiting circulation and slowing the delivery of oxygen and nutrients needed for healing.
Early warning signs of a diabetic foot ulcer may include redness, swelling, warmth, or changes in skin color on the foot. You may notice a callus with dark tissue underneath, drainage on socks, or a wound that doesn’t seem to improve. In some cases, there may be a foul odor, which can indicate infection. Because pain is often absent, visual inspection of the feet becomes extremely important.
Foot deformities, ill-fitting shoes, and prolonged pressure are common triggers for ulcers. Even something as minor as a small blister or cracked skin can progress into an open wound when healing is impaired. Without proper treatment, bacteria can enter the wound, leading to infection that spreads to deeper tissue or bone.
When diabetic foot ulcers are not treated promptly, the consequences can be severe. Infection is one of the most serious risks and may require hospitalization or intravenous antibiotics. In advanced cases, tissue damage becomes irreversible, and amputation may be necessary to protect the patient’s overall health.
This is why early intervention at a specialized wound care clinic is so important. At Bellagio Wound Care, patients with diabetic foot ulcers receive comprehensive evaluations that address not only the wound itself, but also circulation, pressure points, infection risk, and underlying medical conditions. This holistic approach is essential for successful healing.
Advanced treatment options may include professional wound debridement, specialized dressings, offloading techniques to reduce pressure, compression therapy when appropriate, and advanced technologies such as negative pressure wound therapy. Education plays a key role as well, empowering patients to care for their feet properly and recognize signs of trouble early.
Daily foot checks, proper footwear, blood sugar control, and regular medical care are critical steps in preventing diabetic foot ulcers. However, once a wound has formed, home care alone is rarely enough. Prompt evaluation by a wound care specialist can dramatically improve healing outcomes and reduce the risk of long-term complications.
If you have diabetes and notice any changes to your feet — no matter how small they may seem — don’t wait. Early treatment saves limbs and lives. Bellagio Wound Care is committed to providing expert, compassionate care for patients facing diabetic foot wounds, helping them heal safely and regain peace of mind.
REQUEST APPOINTMENT
Follow us on social media!
For people living with diabetes, foot health is more than a comfort issue — it’s a critical part of overall health. One of the most serious and common complications of diabetes is the development of diabetic foot ulcers, open sores or wounds that form due to a combination of nerve damage, poor circulation, and delayed healing.
What makes diabetic foot ulcers especially dangerous is that they often start small and painless, allowing them to go unnoticed until they become severe. Recognizing the early warning signs can help prevent infection, hospitalization, and even amputation.
Diabetes affects the body’s ability to heal in several ways. Over time, high blood sugar levels can damage nerves, a condition known as diabetic neuropathy. This reduces sensation in the feet, meaning cuts, blisters, or pressure points may not be felt at all. At the same time, diabetes can narrow and harden blood vessels, limiting circulation and slowing the delivery of oxygen and nutrients needed for healing.
Early warning signs of a diabetic foot ulcer may include redness, swelling, warmth, or changes in skin color on the foot. You may notice a callus with dark tissue underneath, drainage on socks, or a wound that doesn’t seem to improve. In some cases, there may be a foul odor, which can indicate infection. Because pain is often absent, visual inspection of the feet becomes extremely important.
Foot deformities, ill-fitting shoes, and prolonged pressure are common triggers for ulcers. Even something as minor as a small blister or cracked skin can progress into an open wound when healing is impaired. Without proper treatment, bacteria can enter the wound, leading to infection that spreads to deeper tissue or bone.
When diabetic foot ulcers are not treated promptly, the consequences can be severe. Infection is one of the most serious risks and may require hospitalization or intravenous antibiotics. In advanced cases, tissue damage becomes irreversible, and amputation may be necessary to protect the patient’s overall health.
This is why early intervention at a specialized wound care clinic is so important. At Bellagio Wound Care, patients with diabetic foot ulcers receive comprehensive evaluations that address not only the wound itself, but also circulation, pressure points, infection risk, and underlying medical conditions. This holistic approach is essential for successful healing.
Advanced treatment options may include professional wound debridement, specialized dressings, offloading techniques to reduce pressure, compression therapy when appropriate, and advanced technologies such as negative pressure wound therapy. Education plays a key role as well, empowering patients to care for their feet properly and recognize signs of trouble early.
Daily foot checks, proper footwear, blood sugar control, and regular medical care are critical steps in preventing diabetic foot ulcers. However, once a wound has formed, home care alone is rarely enough. Prompt evaluation by a wound care specialist can dramatically improve healing outcomes and reduce the risk of long-term complications.
If you have diabetes and notice any changes to your feet — no matter how small they may seem — don’t wait. Early treatment saves limbs and lives. Bellagio Wound Care is committed to providing expert, compassionate care for patients facing diabetic foot wounds, helping them heal safely and regain peace of mind.